Other priorities for good health




Topics …
- 6.1 Sleep
- 6.2 Stress management
- 6.3 Dental health
- 6.4 Personal relationships
- 6.5 Choosing the right doctor
- 6.6 What doctors don’t tell you
- 6.7 Skin health
- 6.8 Menopause
- 6.9 Toxins
- 6.10 Vaccinations
- 6.11 Important health documents
6.1 Sleep
Sleep is often sacrificed to squeeze in an extra hour or 2 of productive time. Ironically, this is invariably counter-productive – what is gained in extra waking time, is lost in performance, efficiency and health. In fact, lack of sleep (less than the 7-9 hours for most adult age groups) has an adverse effect on mood, emotional regulation, ability to deal with other people, physical and mental health. It contributes to increased rates of cancer, diabetes, heart disease, weakened immunity, weight gain and Alzheimer’s disease.

Research also reveals that the shorter your sleep, the shorter your life, and different studies show that athletes who get 6 or less hours sleep the night before an event will become exhausted 30% sooner – a powerful “wake up” call.
Personal story – inadequate sleep:
ET, a 29-year-old graphic designer from Melbourne, was routinely getting only 4 to 5 hours of sleep per night, well below the recommended 7-9 hours. Over several months, she noticed increasing fatigue, difficulty concentrating at work and mood swings. She also developed frequent headaches and was getting a cold more often. After a particularly stressful period, she experienced a minor car accident due to a microsleep while driving. Realizing the severity, she consulted her GP who recommended a sleep hygiene routine including consistent bedtimes, reducing screen time before bed, and mindfulness meditation. She also started exercising and didn’t have any coffee after 2 PM. Within weeks, ET’s sleep improved to 7 hours nightly, and her symptoms gradually fell away.
What is needed for good sleep

Consistency is the key to good quality sleep.
This is aided by going to bed at a similar time each night; getting up at the same time each morning; sleeping in a dark room with a reasonably cool temperature; and avoiding screens (phones, tablets and TV) for at least 30 minutes and preferably 1 hour before bed.
Although some studies suggest that avoiding screens does not apply to all people, it seems that most are affected by the blue light emitted by screens which disrupts the human body’s natural sleep signals.
Sleep apnoea
Sleep apnoea occurs when the airway becomes partially or completely blocked during sleep, causing repeated pauses in breathing. These interruptions can happen hundreds of times a night, often without the person realizing it. Each pause triggers a brief arousal from sleep so the body can resume breathing, but this fragmentation prevents deep, restorative rest. Untreated, it can lead to excessive daytime sleepiness, irritability, headaches and difficulty concentrating. If you notice any of these issues or you snore loudly, gasp, choke during sleep or you are overly restless, a visit to the doctor is essential. Over time, sleep apnoea can cause increased risk of high blood pressure, heart disease, stroke and type 2 diabetes.
Personal story – sleep apnoea:
JG, a 54-year-old accountant from Brisbane, had been feeling unusually tired during the day. His wife noticed he sometimes stopped breathing briefly during sleep. After a routine health check, his doctor referred him for a sleep study which confirmed moderate obstructive sleep apnoea. Untreated, JG was at risk of high blood pressure and heart disease. He started using a CPAP machine resulting in better quality sleep. After consistent use, he reported better daytime alertness and improved blood pressure.

Tiredness or fatigue?
Even though these terms are often used interchangeably, they have different causes and different consequences (see table below). Think of tiredness as your body’s natural signal to recharge. Fatigue is more serious and needs to be treated.
| Tiredness | Fatigue | |
|---|---|---|
| Definition | A temporary state of low energy, usually due to exertion or lack of sleep | A persistent, deeper exhaustion that doesn’t resolve with rest |
| Cause | Late night, intense work, physical activity | Chronic stress, sleep disorders, illness, nutritional deficiencies |
| Relief | Usually improves with sleep, hydration or downtime | Often does not improve with rest alone |
| Duration | Short-term | Long-lasting: likely to be fatigue if lasts more than 2 weeks |
| Symptoms | Sleepiness, yawning, mild sluggishness | Brain fog, low motivation, physical heaviness, headaches, weight changes, emotional depletion; trouble staying awake reading, watching TV etc |
| Medical Concern | Rarely serious unless persistent | May signal underlying health issues (e.g. sleep apnoea, depression, thyroid) |
6.2 Stress Management
Stress isn’t always obvious. While we often associate it with feeling overwhelmed or anxious, harmful stress can be quiet and persistent – creeping into daily life without us even noticing.

Meeting deadlines, juggling work and family responsibilities, managing finances, or simply keeping up with all the daily tasks can contribute to chronic stress. Over time, this kind of pressure can adversely affect sleep, digestion, memory, mood/irritability, energy level, immune function and cause an increase in sickness. Ideally, the best way to deal with stress is to remove its source. But, because that’s not always realistic, it’s important to learn how to manage it effectively.
Quick tips for managing stress
- Pause and breathe deeply (see Deep breathing below) when you feel rushed, anxious or overwhelmed
- Build short breaks into your day – even five minutes can help
- Notice physical tension and gently stretch or move
- Keep a simple journal to track mood, sleep, and energy
- Talk to someone – a friend, GP, or counsellor
- Prioritise sleep
- A balanced protein rich diet (see section 2.7 – Diet and Stress).
- Focus on one task at a time
- Mindfulness and meditation (see section 5.3 – Mindfulness).
When to seek help
If you experience any of the following for more than a few weeks, it may be time to speak with your GP or a mental health professional:
- Persistent fatigue or low energy
- Difficulty sleeping or waking up unrefreshed
- Ongoing feelings of sadness, anxiety, or irritability
- Trouble concentrating or making decisions
- Loss of interest in activities you usually enjoy
- Physical symptoms like headaches, digestive issues or muscle tension
Deep breathing
Breathing deeply and slowly calms the body by activating the parasympathetic nervous system, which offsets the effects of stress by counteracting the “fight or flight” mechanism. It does this by reducing cortisol levels, lowering blood pressure and heart rate – thereby reducing anxiety and assisting healing. Deep breathing can also enhance sleep quality, digestion and immune function. It also fosters mental clarity and can help with the management of pain.

One of the more popular deep breathing techniques is called “box breathing” – breathing in deeply (preferably through your nose) for 4 seconds; holding your breath for 4 seconds; breathing out (through your mouth) for 4 seconds and holding for another 4 seconds.
6.3 Dental health
Dental health is far more than just keeping your teeth clean – it plays a vital role in overall physical wellbeing. Poor oral hygiene can lead to gum disease, which is associated with chronic inflammation that does not stay confined to the mouth. It can affect the entire body, contributing to conditions such as cardiovascular disease, diabetes and respiratory infections.

Maintaining good dental hygiene – regular brushing, flossing and dental check-ups – helps reduce systemic inflammation and supports immune function. In this way, dental care becomes a proactive health practice that protects not only oral health but also heart health, metabolic balance and overall resilience.
Further reading: The link between oral health and heart disease
Personal story – the cost of disregarding dental health:
MH, 62, from Newcastle, NSW, thought she was healthy. She walked daily along the foreshore, cooked balanced meals and rarely needed to see a doctor. But she had one blind spot: she avoided going to the dentist for years and thought dental hygiene checkups were waste of money. She even disregarded bleeding gums and convinced herself it was caused by “brushing too hard”. She developed periodontitis (gum disease) which started from an untreated cavity and resulted in a root canal infection and loss of teeth. She became self-conscious about her smile and therefore avoided social outings, which adversely affected her well-being. It also cost her over $7000 over a period of two years to fix the problem.
6.4 Relationships – social connections
Most people underestimate the importance of good relationships and social connections for promoting good health. For example, studies showed that they are helpful for reducing stress, building resilience and even extending life expectancy.
Conversely, chronic loneliness and relationship conflicts can increase the risk of mental decline, a higher risk of Alzheimer’s disease, illness and depression. It can also result in premature death.
Loneliness isn’t about being alone, but feeling alone. Further reading: Health benefits of relationships

Relationship quality matters more than quantity
It’s not about having hundreds of contacts – it’s about having safe, trustworthy and mutually respectful connections. Toxic or chronically stressful relationships can harm health more than solitude.
Mindfulness and relationships
Emotions are fast – they surge before we’ve had time to think, especially when triggered by something unexpected such as a sharp comment or a perceived slight. It’s worse when we’re tired or stressed. Our tolerance shrinks, our reaction time shortens, and we respond in a way that is not helpful. This is often where things unravel – not because of the trigger itself, but because of the reaction that follows.

Mindfulness can help – by reclaiming the space between the stimulus and the response through awareness. It may be necessary to practise this e.g. by listening more intently and pausing before responding; and/or by taking a deep breath in those low-stakes moments when someone interrupts you, or you are irritated by something that was said. It may also help if you recognise your emotion – e.g. anger, hurt, defensiveness – which can make it easier to control the emotion.
6.5 Choosing the right medical practitioner
The right medical practitioner – whether a GP or specialist – can make a big difference to the outcome you get, so it’s very important to ensure that you are seeing the right person. But how do you know if he/she is the right one?
One of the most important criteria is relevant experience in relation to your specific problem. For example, if you need an operation, make sure the surgeon has performed exactly the same procedure many times. Research shows that outcomes improve significantly once a surgeon has done a specific procedure at least 50 times, and preferably 100. For complex surgeries, 200 or more is preferable.
For unusual, complex and/or persistent issues, shopping around is often the answer. Even doctors who specialise in a particular area of medicine don’t necessarily know everything about that area, so you need to ascertain whether they have dealt with your specific problem previously and, if so, how many times.
The right medical practitioner should explain all relevant issues thoroughly, but this does not always happen. So, you need to take the front foot and ask questions: How many times have you performed this particular operation? What are the possible side-effects? Is there anything that you haven’t told me that I should know? What should I do to be proactive?
After your consultation, ask yourself: Did the doctor listen attentively? Did he explain things clearly and check your understanding? Does everything add up?

Personal story
A urologist advised TH, 64, that the increase in his PSA level meant that it was important to do a biopsy “next Wednesday” which involved inserting 20+ needles into his prostate. It didn’t seem right to rush such a procedure based on one blood test. TH decided to get another blood test – his PSA had gone back to normal! When confronted with this, the urologist was defensive and argued that it was standard procedure, although reports from another patient indicate that he is now more careful to avoid recommending an operation based on the result of one blood test, rather than a pattern of results.
If you are not certain that the doctor you have seen is the right one, it is a good idea to get a second opinion. Keep in mind that it is important you feel comfortable that the doctor is not only experienced but is also caring – research shows that patients recover more quickly and cope better when they feel genuinely cared for.
6.6 What doctors don’t tell you

It is not uncommon for people to have an operation without knowing all the potential risks. It is also not uncommon for doctors to fail to advise their patients that being proactive – the right diet, exercise, check-ups, sleep, stress management, etc – can make a significant difference to their future health and quality-of-life. So, as discussed it 6.5 above, you need to ask the right questions.
Personal stories – what doctors haven’t told patients.
- The eye specialist who failed to warn his patient that a cataract operation (that is often used by people who don’t have a serious cataract problem to avoid wearing glasses) has a risk that the retina will become detached, which causes a serious ongoing problem. Incidentally, I am personally aware of this happening to 3 different people.
- The urologist who omitted to tell his patient that the operation on his prostate has a possible risk of incontinence or sexual dysfunction, and that there is a less invasive alternative.
- The patient who suffered debilitating shoulder pain for two years despite consulting different GP’s and specialists only to accidentally find out that the joint was dislocated, with immediate relief when the dislocation was dealt with.
- The patient who reported chronic constipation to different GP’s and specialists for 40 years before a friend suggested trying an off-the-shelf laxative that managed the problem within weeks.
- The doctor who failed to explain the risk of kidney damage from the long-term use of painkillers.
- The general practitioner who failed to advise his patient about the importance of getting a calcium score to determine if he may have a build-up of plaque that could block arteries and cause a heart attack or stroke.
- The cervical spine surgeon who failed to disclose that the patient’s disk had ruptured even though the MRI report (which was not given to the patient) stated that the disk had ruptured.
The last example also demonstrates the importance of getting your own copy of reports including CT scans, X-rays, MRIs, blood tests, etc, and reading them carefully (although sometimes you may need AI to explain in plain English what it means).
It’s also a good idea to ensure that a copy of the letter that your specialist sends to your GP is also sent to you. This avoids the possibility that the specialist has told your GP something in the letter that he didn’t tell you face-to-face, or that you may have overlooked something the specialist mentioned.
The stories go on and on. Perhaps you’ve got one? If you do, we would love to hear from you about it by completing the feedback form or emailing feedback@proactivehealthguide.com.au
6.7 Skin health
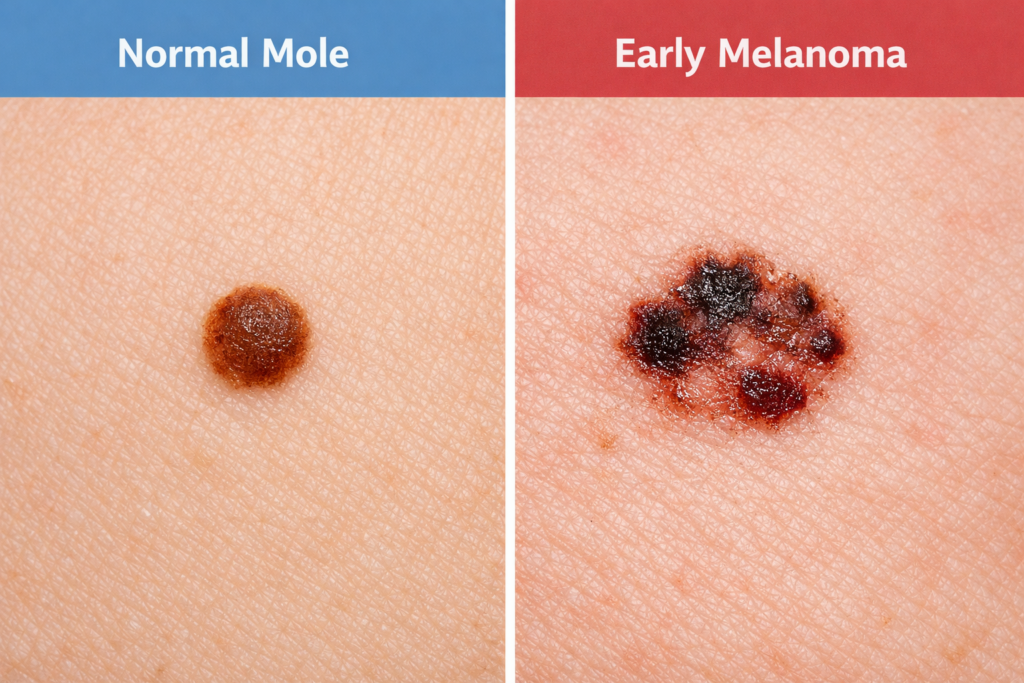
Most Australians know that too much sun can cause skin cancer – melanomas; basal cell carcinomas; squamous cell carcinomas. What’s not widely known is that UV exposure also causes quite a lot of non‑cancer skin problems that can last a lifetime:
- premature ageing – wrinkles, sagging or leathery skin, broken blood vessels.
- mottled skin, uneven pigmentation, sunspots.
- fragile skin that tears and bruises easily; slow healing.
- conditions such as rosacea and some dermatitis.
- reduced immunity – sun exposure weakens the immune layer of skin.
The good news is that they are preventable, and our skin is our first line of defence. It shields us from damage which would otherwise be caused by UV radiation, germs and chemicals. It helps control our temperature and is packed with immune cells that detect infections early and repair damage.
It also plays a role in vitamin D production, microbiome balance and, of course, our appearance which has a significant influence on how we see ourselves – our identity – which in turn influences our self-esteem, motivation, social connection and overall well-being.
People with a positive self-image are more likely to exercise, eat well, develop good habits, pursue goals and engage socially. So, appearance is not superficial. Further reading: Body image https://www.beyondblue.org.au/mental-health/body-image ; Appearance and its effect https://www.mentalhealth.org.uk/explore-mental-health/a-z-topics/body-image.
Most people are aware of the need for sun protection but underrate the importance of taking care of their skin in other ways. The following should all be part of a person’s normal health routine. Further reading: UV Radiation and Your Skin
- Sun protection – SPF 50+; wear a hat, sunglasses and protective clothing.
- Daily care – use gentle cleansers; moisturise regularly, especially after sun exposure.
- Drink water during the day and eat a diet rich in antioxidants
- Lifestyle – avoid smoking and manage stress, which can aggravate many skin conditions.
- Monitor your own skin regularly and get a professional skin checkup every year.

- Avoid smoking and manage stress, which can aggravate many skin conditions.
- Protect fragile skin on arms and hands.
6.8 Menopause
Menopause involves a major hormonal shift with long‑term health implications caused by oestrogen levels falling, which can have an adverse effect on many aspects of health, such as:
- Cardiovascular disease (heart attack, stroke)
- Cognitive decline, especially with early menopause
- Depression, anxiety and chronic sleep problems
- Genitourinary syndrome – dryness, pain, UTIs, incontinence
- Osteoporosis and fractures
- Sarcopenia (muscle loss) and frailty
- Metabolic syndrome – weight gain, insulin resistance, diabetes risk
- Chronic joint pain and inflammation
Many of these risks can be reduced, or prevented, with early management, ideally during perimenopause in the mid-40s. Typically, this involves hormone replacement therapy (HRT) – although it’s not suitable for everyone – in order to relieve hot flushes, sleep problems, and mood changes; protect bone density; reduce fracture risk; improve urogenital symptoms; and support overall wellbeing.

Proactive health practices such as the following are also important:
- Weight‑bearing and resistance exercise
- Adequate calcium and vitamin D
- Avoid smoking and limit alcohol
- Healthy diet rich in whole foods
- Prioritise sleep
- Manage stress
Targeted treatments may also be called for:
- Vaginal oestrogen for dryness, pain, UTIs, and urinary symptoms
- Bone‑specific medications if fracture risk is high
- Sleep and mood support when needed
- Pelvic floor therapy for bladder symptoms
Ongoing monitoring is important:
- Bone density scans (DEXA)
- Cardiovascular risk checks
- Review of symptoms and treatment response
- Screening for metabolic changes
6.9 Toxins
Reducing exposure to everyday toxins is important. Many common household items, such as cleaning products, air fresheners and pesticides, contain chemicals that may affect our physical and mental well-being over time. Gardening, too, often involves fertilizers and herbicides that carry potential risks. Opting for low-tox or natural alternatives, improving ventilation, and safely storing or disposing of hazardous materials are practical steps that help reduce exposure and promote healthier living spaces.

Personal story – garden pesticides:
MM, a 45-year-old landscaper from Perth, developed chronic respiratory issues and skin irritation. Initially, he attributed symptoms to seasonal allergies. After worsening symptoms, he sought medical advice. Tests revealed exposure to herbicides and pesticides used in his work without adequate protective gear. MM was unaware these chemicals could cause health problems. He was advised to use protective clothing, masks, and gloves. With these changes and medical treatment, his symptoms went away after several months. He was lucky – toxins can sometimes lead to long-term health issues.
6.10 Adult vaccinations
Unlike childhood vaccines (such as polio, measles, diphtheria, etc) adult vaccinations are designed to protect against illnesses that become more common and more serious as we age, and our immune systems become less robust. These are listed in the left-hand column of the table below.

It’s important to be aware that acute viral infections such as influenza and COVID‑19 can sharply increase the risk of heart attack and stroke in the weeks following illness but, despite the fact that flu shots are free after the age of 65, 25% of people over this age in Australia do not take advantage of their free vaccine. Chronic infections like HIV, hepatitis C and shingles also elevate cardiovascular risk over the longer term. Vaccination helps reduce both the direct burden of these infections and their associated cardiovascular complications.
| Vaccine | Benefit | Cost (AUD) | Eligibility Notes |
|---|---|---|---|
| COVID-19 | Reduces severity, hospitalisation, and long COVID risk | Free under NIP | Booster schedule varies by age and risk |
| HPV (Human Papillomavirus) | Prevents cervical and other cancers | Free for teens; adults may pay privately | Most effective before sexual activity begins |
| Influenza (Flu) | Reduces risk of severe flu, hospitalisation, and complications | Free for over 65s, pregnant women, First Nations people | Annual vaccination recommended |
| Pneumococcal | Protects against pneumonia, meningitis, and bloodstream infections | Free for over 70s and high-risk groups | Booster may be needed depending on age and health |
| RSV | Protection against pneumonia and bronchitis; stops exacerbation of COPD and asthma | Not yet widely available on national health | Recommended for 60+ and those with chronic health conditions |
| Shingles (Zoster) | Prevents painful rash and nerve damage; may reduce risk of post-herpetic neuralgia | Free for adults aged 70+ | Available under National Immunisation Program (NIP) |
| Whooping Cough (Pertussis) | Protects infants and vulnerable adults from severe respiratory illness | Free for pregnant women and some carers | Adults may need boosters every 10 years |
6.11 Important health documents
The availability of your health records and other important health documents – such as those referred to in the following paragraph – may be critical to your future health needs. For example, if you are injured or suddenly fall ill away from home, and need to be treated urgently, your medical records could make a significant difference to the outcome of your treatment. You don’t carry them around with you so it’s important to have them accessible online.
My Health Record provides a government-managed platform for storing personal health information in one central location that can be accessed by authorised healthcare providers. It can include medications, allergies, test results, immunisation history, etc. You can control who sees your information and update privacy settings at any time. You will need to authorise your medical providers to upload your medical records: My Health Record.

Other documents, such as the Appointment of an Enduring Guardian and an Advance Health Care Directive, are “just in case” documents, but it doesn’t make them less important. For example, if you have a life changing accident or illness, you may be in a coma and not be able to make a decision yourself.
It is therefore necessary to have a document which authorises someone to make those decisions on your behalf – a “guardian”– and specifies what you want to happen.
An Advance Health Care Directive is important if the Guardian you have appointed is not around at the time a decision needs to be made. This also needs to be given a lot of thought and you may want to consult a solicitor about this to get the wording right. Further reading: Advance Care Directive.
A lot of care needs to be taken in ensuring that the terms of the appointment reflect exactly what you want. For example, you may want to specify in advance that you do not want to be kept on life support if there is no prospect of your recovering from a serious accident, which may involve permanent brain damage, quadriplegia, etc. This is a different document to an Enduring Power of Attorney that enables someone to make financial decisions on your behalf if you are not able to.